Hospital air filtration systems are critical components of modern healthcare facilities, playing a vital role in preventing the spread of airborne infections and maintaining a sterile environment. These systems aren't merely about cleanliness; they’re about patient safety, staff wellbeing, and overall public health. The need for sophisticated air purification has become increasingly apparent in light of global health crises and the rising prevalence of antimicrobial resistance.
Globally, the demand for advanced hospital air filtration systems is growing, driven by increasing healthcare expenditures, stringent regulations regarding indoor air quality, and a heightened awareness of the dangers posed by airborne pathogens. Organizations like the World Health Organization (WHO) and ISO are continually updating guidelines and standards to promote best practices in air purification within healthcare settings. Investing in these systems is not just a best practice, but a necessity for responsible healthcare provision.
The effectiveness of these systems is paramount, impacting patient recovery times, reducing healthcare-associated infections (HAIs), and protecting vulnerable populations. From operating rooms to intensive care units, hospital air filtration systems are integral to providing a safe and effective healing environment. Understanding their intricacies and implementing the right solutions is essential for any modern healthcare institution.
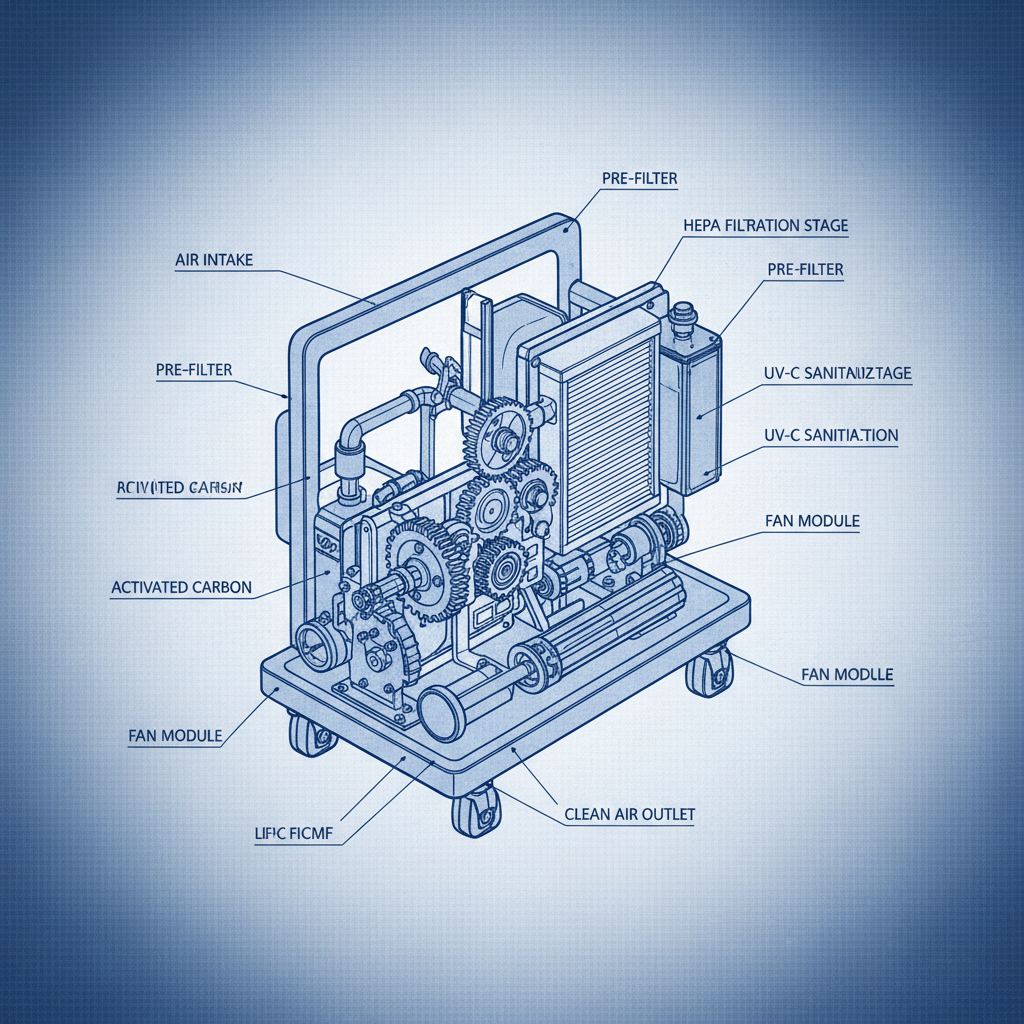
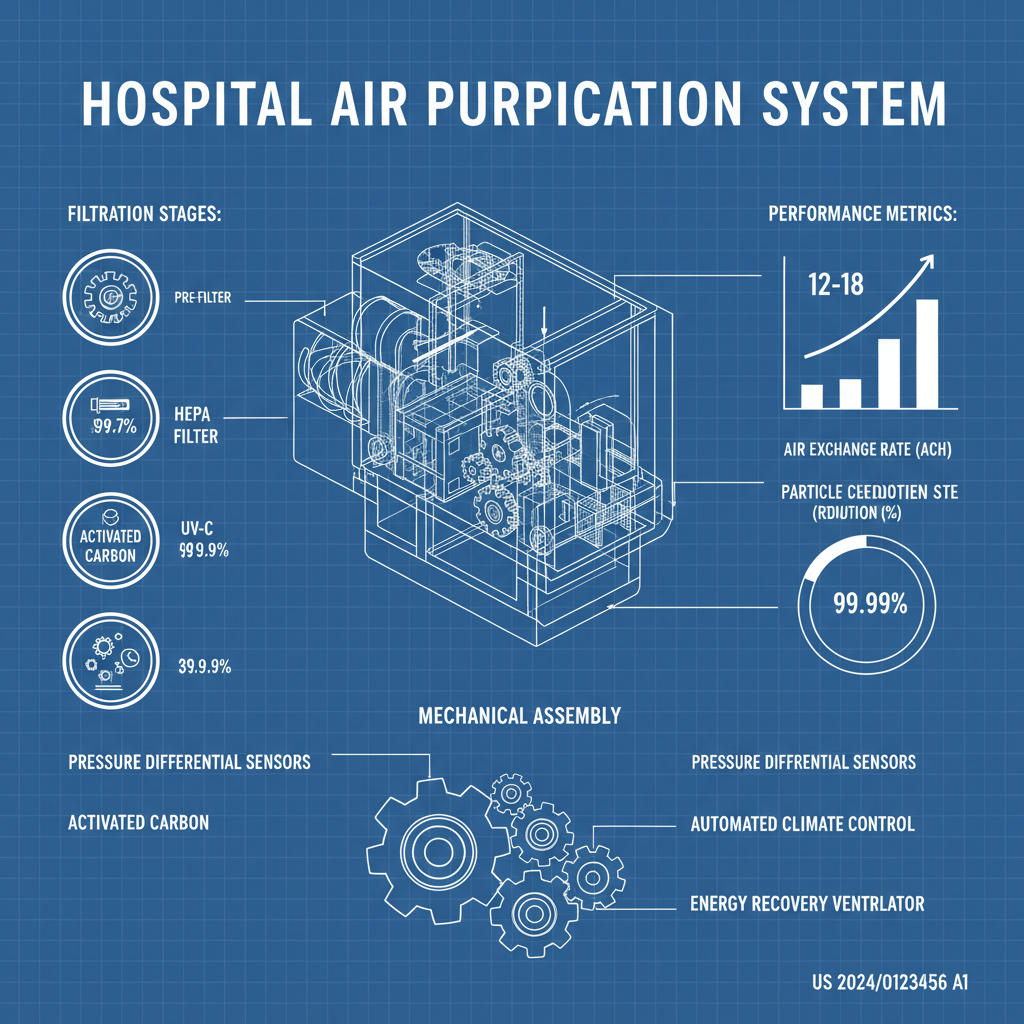
Hospital air filtration systems are essential for removing airborne contaminants, including bacteria, viruses, fungi, dust particles, and volatile organic compounds (VOCs). The consequences of inadequate air purification can be severe, leading to increased rates of HAIs, compromised immune systems, and prolonged hospital stays. Effective hospital air filtration is therefore a cornerstone of patient care.
The complexity of modern hospitals necessitates sophisticated filtration strategies. Different areas require varying levels of purification, from operating theaters demanding ultra-clean air to general wards needing consistent contaminant removal. The selection and implementation of the right systems directly impact the health and safety of patients, staff, and visitors.
Hospital air filtration systems encompass a range of technologies designed to remove pollutants from the air circulating within healthcare facilities. These systems commonly utilize High-Efficiency Particulate Air (HEPA) filters, which are capable of trapping 99.97% of particles 0.3 microns in diameter. However, modern systems often incorporate additional layers of filtration, such as pre-filters, activated carbon filters, and ultraviolet germicidal irradiation (UVGI).
The core function is to provide a consistent supply of clean, filtered air, minimizing the risk of airborne transmission of infectious diseases. This is particularly crucial in areas where immunocompromised patients are treated or invasive procedures are performed. The connection to humanitarian needs extends to field hospitals and emergency response scenarios, where maintaining air quality is even more challenging.
Beyond removing particles, advanced systems also address gaseous pollutants and odors, creating a more comfortable and therapeutic environment. The integration of smart sensors and automated controls allows for real-time monitoring and adjustment of filtration levels, optimizing performance and energy efficiency.
Durability is a critical factor. Hospital air filtration systems must withstand continuous operation and maintain consistent performance over an extended lifespan. Filters need to be robust and resistant to clogging, requiring minimal maintenance and replacement. The longevity of the system directly impacts the total cost of ownership.
Scalability is also paramount. Hospitals come in various sizes and configurations, and their air filtration needs change over time. Systems must be adaptable and expandable to accommodate growth, renovations, or changing patient demographics. A modular design allows for easy upgrades and modifications.
Cost efficiency, encompassing both upfront investment and ongoing operational expenses, is a key consideration. While high-performance systems may have a higher initial cost, they often result in lower long-term costs through reduced maintenance, improved energy efficiency, and fewer HAIs.
Filter efficiency, measured by MERV (Minimum Efficiency Reporting Value) rating, determines the size of particles the system can capture. HEPA filters are the gold standard, but other filter types offer varying levels of protection.
Hospital air filtration systems are employed in a wide range of healthcare settings, including operating rooms, intensive care units (ICUs), isolation wards, laboratories, and pharmaceutical manufacturing areas. Each application demands specific filtration requirements tailored to the potential contaminants and risk levels.
In post-disaster relief operations, mobile hospital air filtration systems are crucial for establishing temporary healthcare facilities with safe and controlled air quality. These systems can be rapidly deployed to provide immediate protection against airborne hazards.
The benefits of investing in high-quality hospital air filtration systems are multifaceted. Reduced HAIs translate to lower treatment costs, shorter hospital stays, and improved patient outcomes. A safer environment also boosts staff morale and reduces absenteeism. Furthermore, compliance with stringent regulatory standards can avoid costly penalties.
From a sustainability perspective, efficient filtration systems can lower energy consumption and reduce the need for frequent filter replacements, minimizing environmental impact. The long-term value extends beyond cost savings to encompass improved public health and a strengthened reputation for the healthcare institution.
Several promising trends are shaping the future of hospital air filtration systems. These include the integration of advanced sensors and artificial intelligence (AI) for real-time monitoring and predictive maintenance. Nanotechnology is being explored to create filters with even greater efficiency and selectivity.
The development of more sustainable filter materials, such as biodegradable or recyclable options, is also gaining momentum. Furthermore, advancements in UVGI technology are leading to more effective and energy-efficient disinfection solutions. These innovations promise to enhance the performance and sustainability of hospital air filtration systems.
One of the primary challenges is the high cost of maintaining and replacing filters, especially HEPA filters. Innovative solutions include developing filters with longer lifespans, utilizing pre-filtration systems to extend filter life, and implementing automated filter monitoring systems.
Another challenge is ensuring adequate ventilation and air distribution within complex hospital layouts. Computational fluid dynamics (CFD) modeling can be used to optimize airflow patterns and identify areas where filtration needs to be improved.
Addressing the issue of airborne transmission of drug-resistant organisms requires a multi-faceted approach, including enhanced filtration, improved ventilation, and rigorous infection control protocols. Collaboration between engineers, healthcare professionals, and regulatory agencies is essential to overcome these challenges.
| Challenge | Impact on Hospital Operations | Proposed Solution | Implementation Cost (1-10) |
|---|---|---|---|
| High Filter Replacement Costs | Increased operational expenses, budget strain | Extended-life filters, pre-filtration systems | 6 |
| Inadequate Air Distribution | Uneven air purification, hotspots for contamination | CFD modeling, airflow optimization | 7 |
| Resistance to Drug-Resistant Organisms | Increased risk of HAIs, prolonged patient stays | Enhanced filtration combined with infection control | 8 |
| Maintaining System Performance | Decreased effectiveness over time, compromised air quality | Automated monitoring and predictive maintenance | 5 |
| Energy Consumption of Systems | High utility bills, environmental impact | Energy-efficient filters and system controls | 4 |
| Compliance with Regulations | Risk of penalties, reputational damage | Regular system audits and upgrades | 6 |
The lifespan of a HEPA filter varies based on usage and air quality conditions, but generally ranges from 6 to 18 months. Frequent monitoring of pressure drop across the filter is crucial to determine when replacement is needed. Ignoring this can reduce system efficiency and compromise air quality. Regular filter changes are a fundamental component of maintaining optimal hospital air filtration systems performance.
Assessing adequacy involves several factors. Regular air quality testing should be conducted to measure particle counts and identify potential contaminants. A qualified HVAC engineer can perform a system assessment to ensure it meets relevant standards and regulations, such as ASHRAE guidelines. Furthermore, consider the specific needs of your facility, such as the presence of immunocompromised patients or high-risk procedures.
Both HEPA (High-Efficiency Particulate Air) and ULPA (Ultra-Low Penetration Air) filters remove particulate matter, but ULPA filters are even more efficient. HEPA filters capture 99.97% of particles 0.3 microns in size, while ULPA filters capture 99.999% of particles of the same size. ULPA filters are typically used in applications requiring the highest levels of cleanliness, such as semiconductor manufacturing and critical surgical environments.
Several strategies can lower energy consumption. Using variable frequency drives (VFDs) on fans allows airflow to be adjusted based on demand. Implementing a robust preventative maintenance program ensures optimal system efficiency. Upgrading to energy-efficient filters and considering demand-controlled ventilation (DCV) can further reduce energy usage. Regular system audits can identify areas for improvement.
Ultraviolet Germicidal Irradiation (UVGI) is an effective method for disinfecting air by using ultraviolet light to kill microorganisms. It's often used in conjunction with filtration systems to provide an additional layer of protection. UVGI can be applied to both air and surfaces, helping to reduce the spread of airborne pathogens. Proper installation and maintenance are crucial for UVGI effectiveness.
Look for a vendor with a proven track record in healthcare, a strong understanding of regulatory requirements, and a commitment to innovation. Consider their service capabilities, including installation, maintenance, and support. Check references and ensure they offer customized solutions tailored to your facility's specific needs. Choosing a reliable vendor is crucial for long-term success.
Hospital air filtration systems are no longer simply an amenity, but a fundamental requirement for providing safe and effective healthcare. From mitigating the spread of infectious diseases to creating a more comfortable environment for patients and staff, these systems play a critical role in protecting public health. Investing in advanced air purification technologies is an investment in the wellbeing of the community.
Looking ahead, continuous innovation in filter materials, sensor technology, and AI-driven controls will further enhance the performance and sustainability of these systems. By proactively addressing the challenges and embracing emerging trends, healthcare facilities can ensure they are equipped to meet the evolving demands of a rapidly changing world. Visit our website at www.meshmachinery.com to learn more about our hospital air filtration solutions.


